Screen Early to Detect Cancers, Experts Urge | China Daily
2024-01-01

Only 20 to 30 percent of cancer cases have genetic links. The majority are due to lifestyle, diet, and toxic environment. Experts urge elderly screening for early detection. There is a significant survivability gain from timely medical intervention via screening. Cancers may not manifest physically until too late. Wang Yuke reports from Hong Kong.
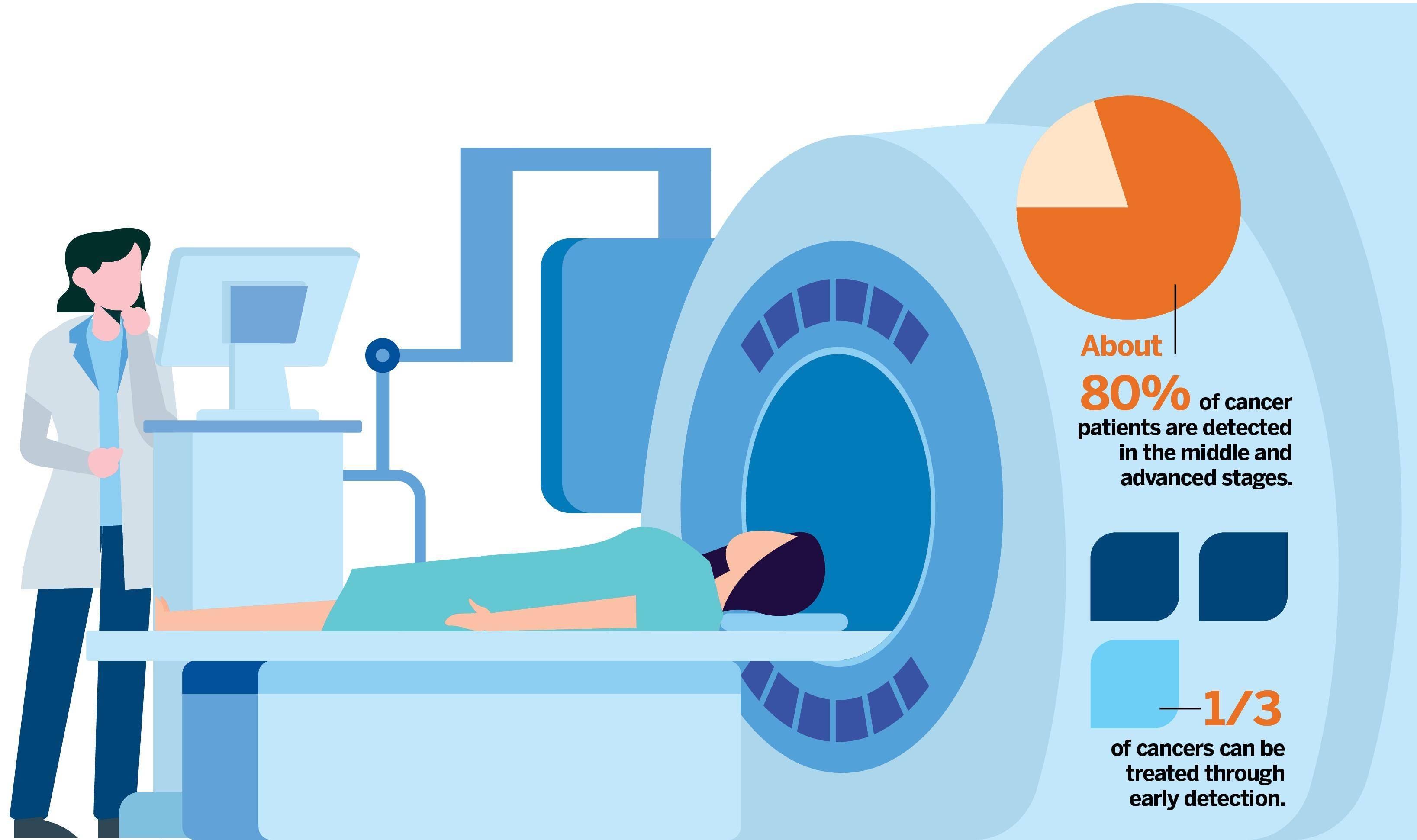
INFOGRAPHICS: DONG KAI, MOK KWOK-CHEONG
It is popularly believed that cancers are hereditary. But 70 to 80 percent of cancer cases have no evident family histories. The vast majority of “sporadic cancer” is attributed to lifestyle, diet, and environmental factors. More disciplined individual lifestyle and location choices can reduce the incidences of cancers. Direct genetic hereditary links have been statistically confirmed for ovarian, breast, colon and rectal cancers.
The World Health Organization defines cancer as transforming normal cells into tumor cells, in a multistage process, from a precancerous lesion to a malignant tumor. The WHO says “30 to 50 percent of cancers can be prevented by avoiding risk factors and implementing existing evidence-based prevention strategies”. Zhu Shida, vice-president of Precision Medicine at BGI, one of the world’s leading genome research organizations, adds that many cancers are predictable, preventable, and curable if diagnosed early.
Theoretically, most cancers can be detected in early stages because cell-free DNA, which exhibits genetic and epigenetic alterations of cancers, is released into the blood as well as other body fluids and therefore can be captured, Zhu says. Carrying molecular characteristics, including somatic mutations and methylation alterations, the cell-free DNA promises an early reliable biomarker for cancer.
Victims unaware
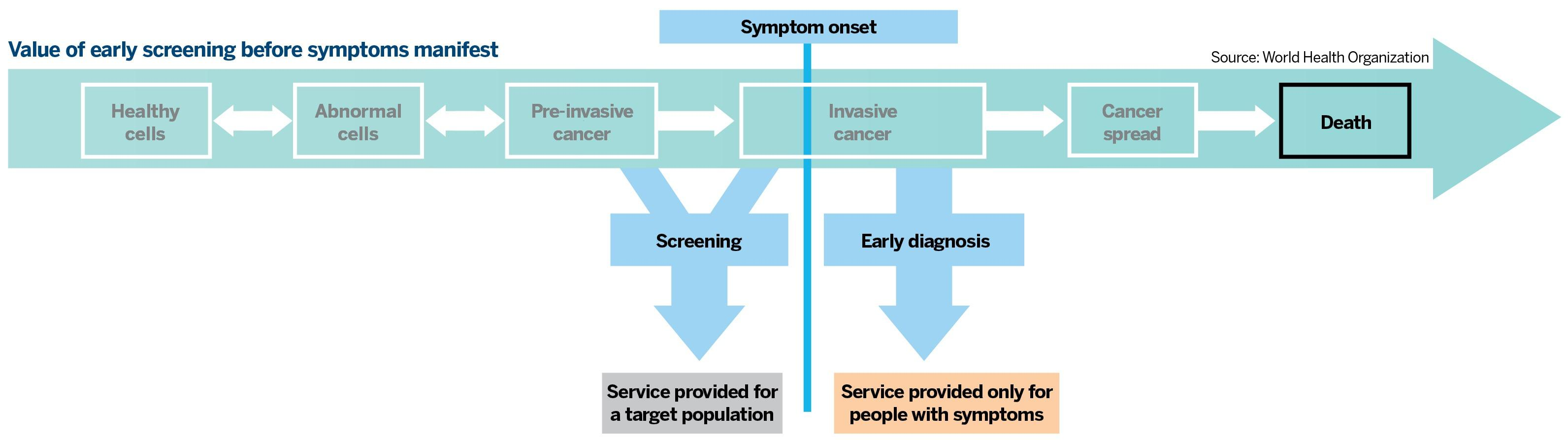
Even though the cell-free DNA can be detected early via medical screening, it may not make its presence felt through symptoms till much later, so people don’t feel the need to screen or volunteer for examination, argues Zhu. That may be too late in many cases.
It takes years for malignant tumors to manifest in imaging, such as CT (computed tomography), X-rays, and MRI (magnetic resonance imaging). The accumulation of either driver mutations or passenger mutations in the genome of one cell implants the seed for the rampant proliferation and growth of bad cells before they become very visible. That may take two to 10 years, depending on the type of cancer, explains Zhu.
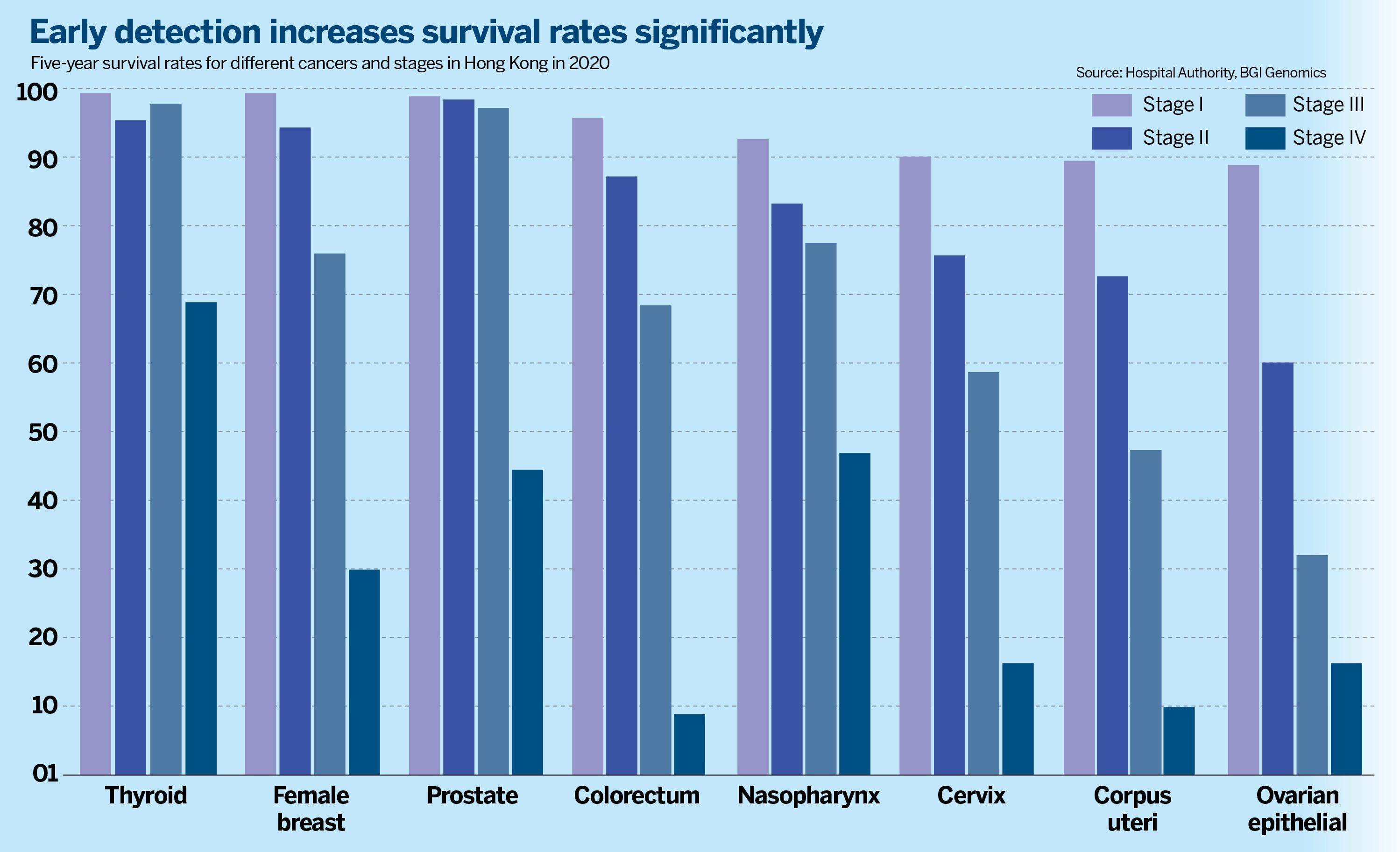
The correlation between preventive screening and early diagnosis translates into improved chances for survival. The survival rate contrast between early diagnosis and the advanced phases is very significant. Take prostate cancer cases in Hong Kong in 2020. The five-year survival rate was very high (greater than 97 percent) in Stage I to III, while it sank to 45 percent in Stage IV, according to the Hospital Authority records.
Early detection and diagnosis is life-changing for patients, leading to timely medical intervention to stop or delay the invincible metastatic spread of the cancer. Zhu cites an experiment by Netherlands scientists published in 2020: The incidences of lung cancer were 5.58 and 4.91 cases per 1,000 person-years in the screening group and the control group respectively, while the mortality was 2.50 deaths and 3.30 deaths per 1,000 person-years respectively.
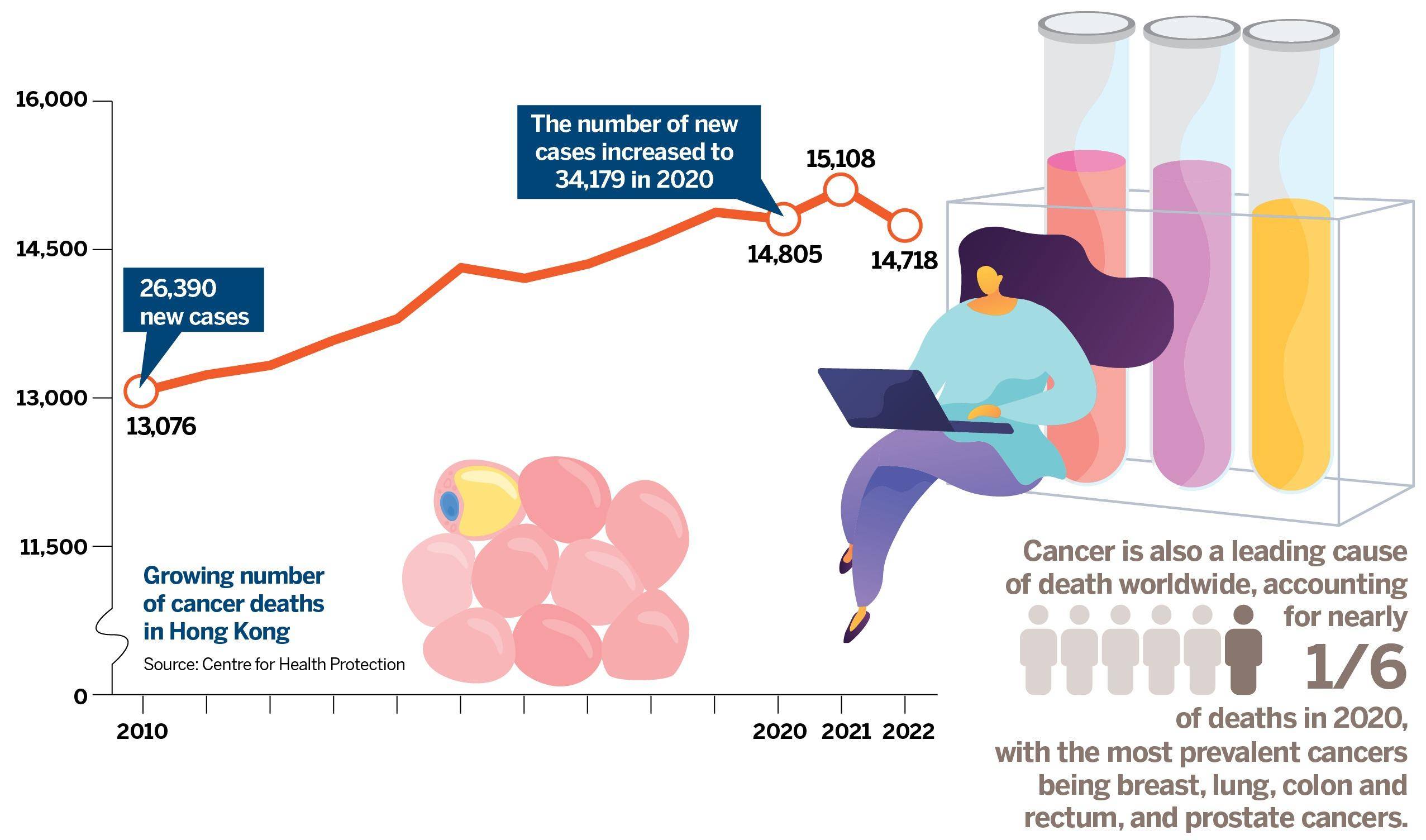
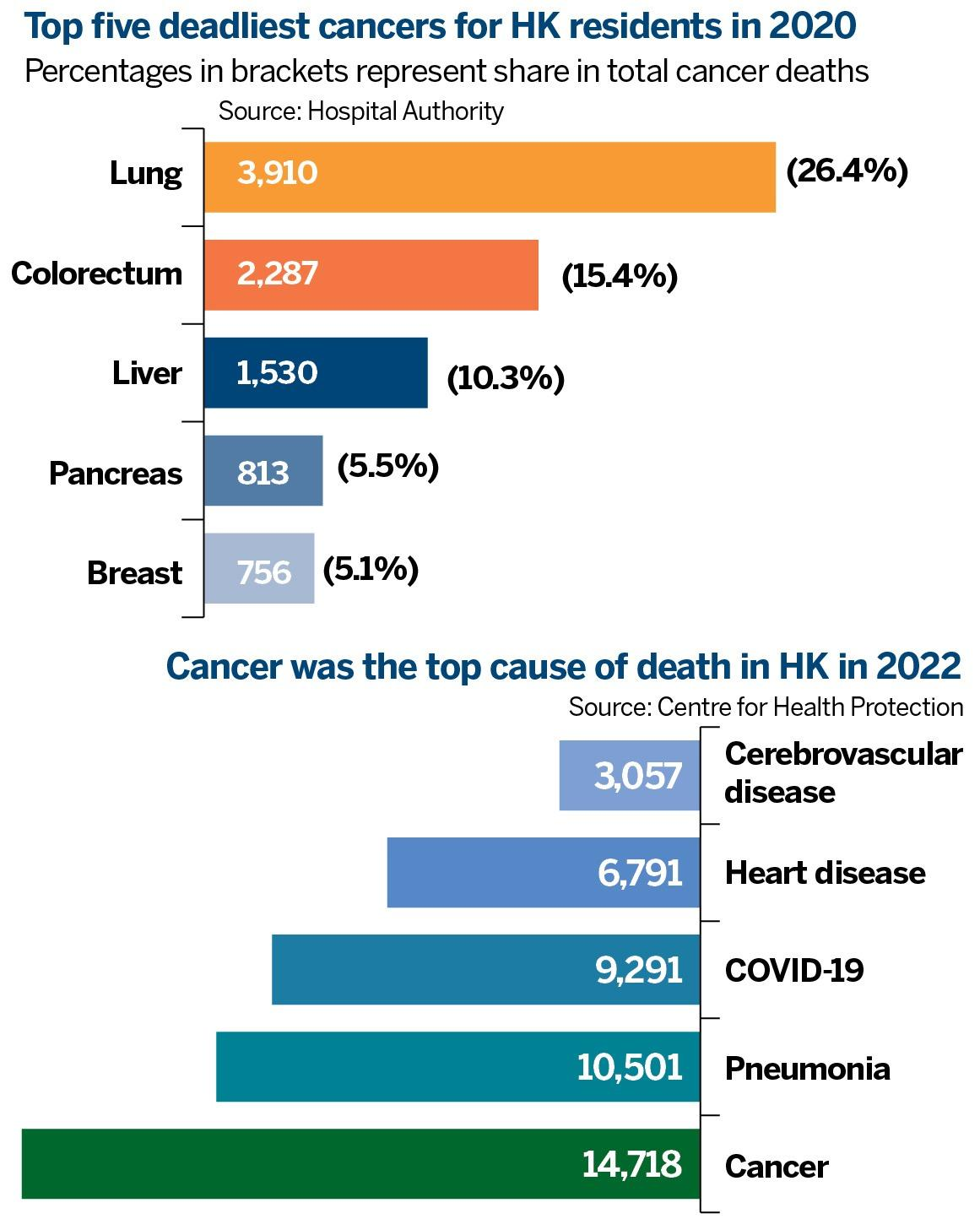
Worldwide, an estimated 19.3 million new cancer cases and 10 million cancer deaths were recorded in 2020. Half of all cases and 58.3 percent of cancer deaths occurred in Asia, where 60 percent of the global population lives. If this trend continues, there will be 28 million new cases each year by 2040, according to the Global Cancer Statistics 2020.
Breast and lung cancers are the most common cancers worldwide, responsible for 12.5 percent and 12.2 percent of the total number of new cases respectively diagnosed in 2020. Colon cancer affected 1.9 million, accounting for 10.7 percent of new cases, reports World Cancer Research Fund International.
The HA tracked cancer mortality over the past decade rising at an annual rate of 1.2 percent. There were 14,805 cancer deaths in 2020, accounting for 29.2 percent of all deaths in Hong Kong.
Life span challenge
With the advances in drugs to keep patients living beyond their natural span, we face a dilemma: Should mere survival, or quality of life, be society’s goal in senior years? There is increasing focus on “health span” as opposed to “life span”. To be kept alive but suffering aches, pains, immobility, and memory loss seems neither useful nor noble.
Affordable screening 2025
The initial Presight tests will be focused on liver and lung cancer, to be made commercially available on the Chinese mainland and in Hong Kong in 2025. The prevalence and affordability of colonoscopies could be the best low-hanging fruit reached by people prone to colorectal cancer, which has indeed paid dividends in reducing the cancer incidences and enhancing likelihood of five-year survival, notes Zhu. Colonoscopies can prevent the cancer stage by nipping the detected polyps in the bud, he adds.
Nevertheless, an endoscopy is far from a panacea because it has a “low patient throughput”. Each endoscopy unit can only perform a limited number of colonoscopies per day. “The resources are barely sufficient to cover 6 million elderly people (in China who are susceptible to colorectal diseases).” The procedural quota is a daunting constraint to overcome.
Despite the WHO’s “Guide to Cancer Early Diagnosis” since 2017 and the National Comprehensive Cancer Network’s up-to-date equivalent, both urging prioritizing of cancer screening for cancer prevention policy implementation, Zhu doubts that it has moved governments’ health care policies as “they may not have enough resources and motivation” to align their policies accordingly.

Subsidized testing
Some governments have taken small steps to approach it. Singapore has taken the initiative to subsidize its citizens for screening, so that each visit costs $5 or less. The program covers common types of cancer as well as chronic diseases, benefiting populations aged 18 to 50 and above. Hong Kong has introduced a Colorectal Cancer Screening Programme, subsidizing asymptomatic Hong Kong residents between 50 and 75 with screening tests every two years.
The fecal test is free. If a further colonoscopy is needed, the resident pays less than HK$1,000 ($128), one-eighth of the standard cost as the special administrative region government offers substantial coverage. Screening for cervical and breast cancers are also available. But other types of cancer detection are not similarly available for reasons of specific screening criteria. 
Martin Wong, professor of the Jockey Club School of Public Health and Primary Care at CUHK, with a specialization in cancer screening and prevention of chronic diseases, says screening methods can be subsidized and encouraged only if they meet all Wilson and Jungner screening criteria.
 That includes: recognizable latent or early symptomatic stage of the cancer, an adequate understanding about the natural course of the cancer’s development, and scientific reliability and cost-effectiveness of the screening technology.
That includes: recognizable latent or early symptomatic stage of the cancer, an adequate understanding about the natural course of the cancer’s development, and scientific reliability and cost-effectiveness of the screening technology.
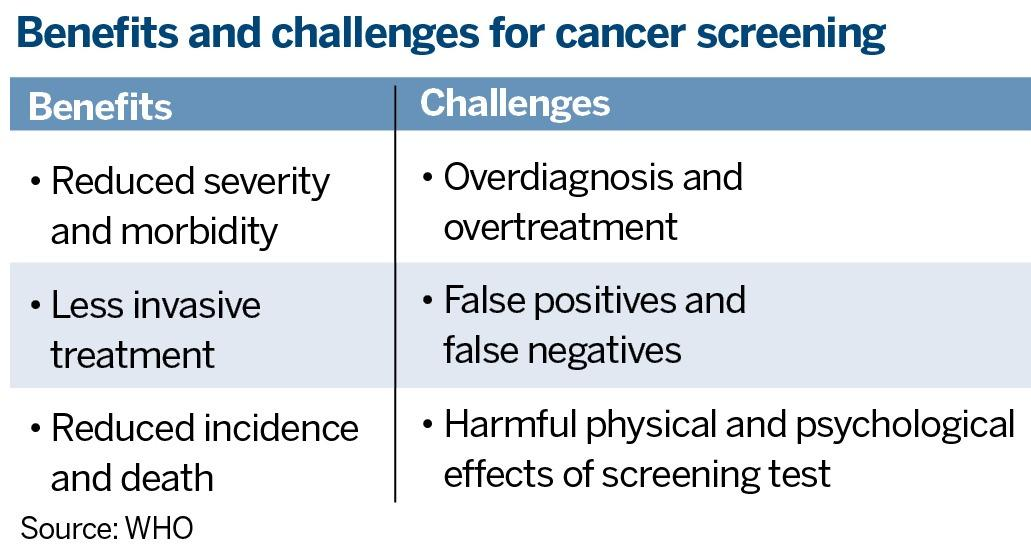
“Screening methods available for lung cancer, pancreas cancer, brain cancer, … for example, are yet to meet the criteria. Some screenings remain controversial as they do more harm than good,” Wong says.
Some screening inventions have unacceptable glitches and inadequate resources necessary for easy availability. Low-dose CT, for instance, is recognized for its growing role in early detection of lung cancer, promising a 20 percent reduction in mortality. Nevertheless, false positives and complications are rife in clinical trials, and facilities are far from enough to meet mounting demands, Wong adds.
AI to help?
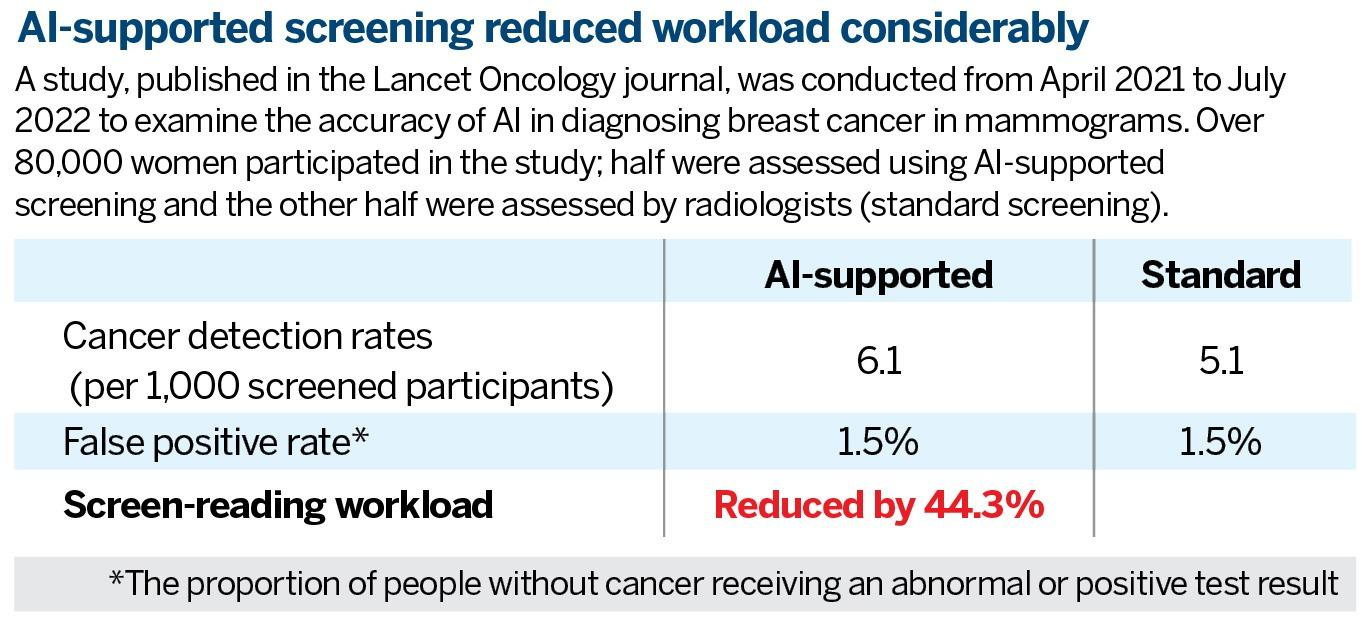
Human marginal errors are inevitable in analysis and judgment because of fatigue and oversight, which is manifested in cancer screening. “False negatives” are not uncommon, resulting in delayed diagnosis, acknowledges Wong. The promise of faster, more reliable screening with artificial intelligence is clear, but the advances are not mature yet to prevent misreading cancer screening.
Distinguishing abnormal tissues and lesions from normal zones requires pattern recognition, which is what computers are good at. European countries are ahead of the curve in this emerging area, with consistently positive preliminary results.
Risk-stratification models
Ranjit Manchanda is leading the effort to develop risk-stratification modeling to allocate screening resources to high-risk populations. Causes for cancer are complex and myriad but largely the result of unhealthy lifestyles and excessive exposure to cancer-inducing environmental substances, says Manchanda, a professor at Queen Mary University of London, whose research focus is on targeted precision prevention. The fact that humans live longer also adds to cancer incidents, he adds.
“Any screening strategy has to balance harms and benefits, factoring the false positives and consequences of unnecessary interventions,” admits Manchanda, who is advocating for and piloting risk-stratification models. Risk stratification is considered to be a feasible short-cut to “targeted” screening and effective cancer prevention.
Apart from the existing and continuing risk-stratification studies for breast cancer, Manchanda also leads a pilot study for ovarian cancer. “We have published data showing the potential cost-effectiveness and impact of population testing for high-risk cancer genes, including across high-income and upper-middle-income countries, including China,” says Manchanda.
“We are about to start a new study next year PROTECT-C (population-based germline testing for early detection and cancer prevention), which tests the general population — women above 18 — for a list of cancer genes associated with breast, ovarian, womb and bowel cancer, as well as providing personalized risk assessment for breast and ovarian cancer, to identify higher-risk individuals who can benefit from targeted screening and preventive interventions,” he adds.

What's next
Make the public aware that 70 to 80 percent of cancers can be detected before symptoms by early screening.
Accelerate screening technologies and subsidize target groups to access.
Use big data to pattern target groups for reliable personalized risk assessment.
Employ AI technologies to help specialists diagnose screening more reliably and speedily.
Remind residents that a healthy lifestyle, safe diet, and outdoor exercise are vital. Avoid toxic environments.
First published: China Daily